Introduction
An ankle sprain can lead to ongoing ankle instability, causing repeated sprains and a feeling of the ankle “giving way.” In cases where non-operative treatments have been ineffective, ankle lateral ligament reconstruction, also known as the Broström procedure, can provide a stable ankle. Discover how this surgical procedure can help restore stability to your ankles and improve your quality of life.
What is ankle lateral ligament reconstruction?
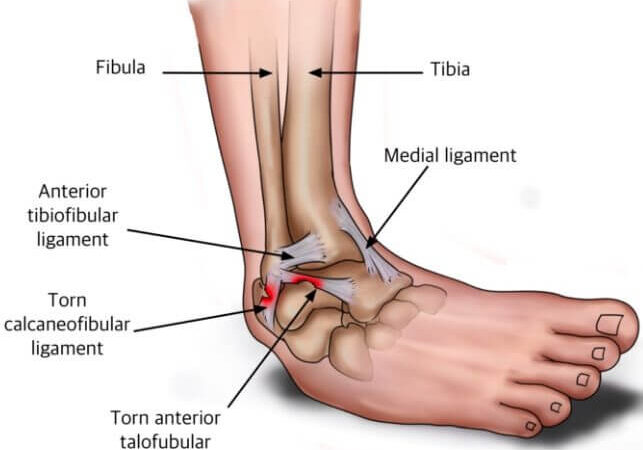
An ankle sprain occurs when the ligaments on the outside of the ankle are injured, often by rolling or twisting the ankle. While most ankle sprains heal with self-care and physiotherapy, a small percentage of patients experience ongoing ankle instability. This instability can be addressed through ankle lateral ligament reconstruction, a surgical procedure that involves reconstructing the damaged ligaments on the outside of the ankle.
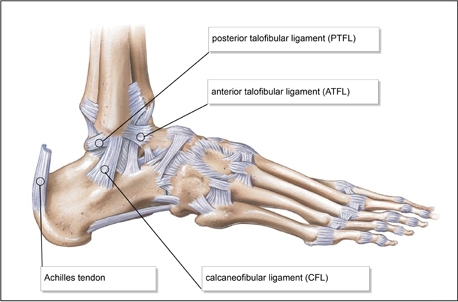
Ankle lateral ligament reconstruction, commonly referred to as the Broström procedure, is typically recommended as a last resort when non-operative treatments have been exhausted and the symptoms of ankle instability persist. Before considering surgery, it is essential to explore conservative treatment options under the guidance of a healthcare professional.
The Procedure and What to Expect
Performing Ankle Lateral Ligament Reconstruction
Ankle lateral ligament reconstruction is usually performed under general anesthesia, although regional or spinal anesthesia may also be used. The surgical procedure involves making a small incision (approximately 5cm) on the outside of the ankle. Plastic anchors with attached stitches are then placed into the bone. The damaged ligaments are meticulously tightened and reattached to the bone. In some cases, an artificial tape may be utilized to reinforce the reconstruction. Ankle arthroscopy may also be performed concurrently with the lateral ligament reconstruction.
Once the surgery is complete, the incision is closed with stitches, and local anesthetic is administered to alleviate pain in the initial hours after the procedure. A temporary plaster or cast will be applied to support the ankle during the initial healing phase.
Mr Mike Barrett uses the Arthrex Fibretak DX suture anchors, below is a video demonstrating this technique. In a small number of patients this is augmented with the internal brace device which is also demonstrate in this video.
Risks and Complications
Understanding the Risks
As with any surgical procedure, ankle lateral ligament reconstruction carries certain risks, both related to the anesthesia and the surgery itself. During your pre-surgical consultation, the risks will be thoroughly explained to you. Below are some potential risks associated with the procedure:
- Swelling: Post-surgery swelling is normal and can take more than six months to fully subside.
- Reconstruction Failure: There is a small chance that the reconstructed ligaments may fail, requiring additional surgery. Adherence to a rehabilitation program can help minimize this risk.
- Nerve Injury: While rare, there is a small risk of nerve damage or stretching during the operation, which may result in temporary numbness.
- Infection: Infections are infrequent, but in some cases, the wound may become infected, necessitating further treatment or surgery.
- Blood Clots: Ankle surgery carries a small risk of blood clots in the leg or lung. Precautions are taken to minimize this risk, but it cannot be completely eliminated.
- Chronic Regional Pain Syndrome: A small proportion of patients may develop chronic regional pain syndrome after foot and ankle surgery, characterized by prolonged pain, swelling, and sensitivity. Consultation with a pain consultant may be required in such cases.
Post-Operative Care and Recovery
Your Road to Recovery
Post-surgery, most patients can go home on the same day, while some individuals with underlying medical conditions may require an overnight hospital stay. During the first two weeks, it is advised to avoid putting weight on the operated leg. Crutches will be provided to assist with mobility. Elevating the leg and keeping the cast or plaster dry are crucial in the initial weeks to reduce swelling and promote wound healing. Consider using a waterproof cover, such as the ones available at www.limboproducts.com.
Two weeks after the surgery, you will have a follow-up appointment in the outpatient clinic. The wound will be checked, stitches removed, and a surgical boot will be provided, allowing you to gradually put weight on your operated leg. The surgical boot should be worn continuously for the next four weeks. A six-week follow-up appointment will monitor your progress, and you may transition into supportive footwear recommended by your healthcare provider. Specialized physiotherapists will guide you through a rehabilitation program to regain ankle strength and balance. The final outpatient appointment is typically scheduled three months after the surgery.
Return to Work, Driving, Activity, and Travel
Resuming Daily Activities
Returning to work will depend on the nature of your job. If you have a sedentary, desk-based job and can elevate your foot, you may be able to return to work two weeks after surgery. However, physically demanding jobs may require a longer recovery period.
Driving can commence when you can walk comfortably in your regular footwear. It is important to ensure you can safely make an emergency stop, as your insurance coverage may be affected otherwise. Gradually reintroduce driving by starting with short distances and practicing in safe conditions.
Follow your surgeon’s guidance and consider individual circumstances, such as driving an automatic car in the case of left leg surgery.
Promoting Recovery and Wellbeing
Supporting Your Recovery
Maintaining a healthy lifestyle can contribute to a smoother recovery and enhance the success of your surgery. A balanced diet, regular exercise, and refraining from smoking can all positively impact your healing process. Taking vitamin C supplements for six weeks before and after surgery may also be beneficial and can be obtained from local pharmacies or supermarkets.
If you have any concerns about your overall health, well-being, or specific lifestyle choices, it is recommended to discuss them with your general practitioner (GP). Your GP can provide advice and guidance on various options available to support your well-being.
Conclusion
We hope this comprehensive guide has addressed your questions regarding ankle lateral ligament reconstruction. Should you have any further inquiries, our medical and nursing staff are available to provide you with the necessary assistance and clarification. Your well-being and recovery are our utmost priority.
Useful links:
https://www.bofas.org.uk/patient/patient-information/ankle-instability
Last modified: June 22, 2023